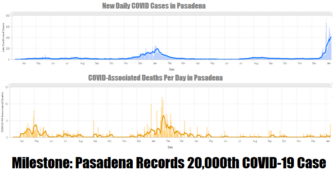
With COVID-19-positive patient count still climbing daily at Huntington Hospital, on Wednesday Pasadena reported four COVID-19-Associated deaths and 424 confirmed new cases, which pushed the city past 20,000 cumulative cases since the pandemic began.
The city’s public health department is still two days behind in reporting. The new information covers through Monday of this week.
In reporting the deaths city spokesperson Lisa Derderian said “three passed away this month and one expired at the end of November 2021. Two were fully vaccinated but had major underlying health conditions. Ages ranged from 65-104 years old — which is our oldest death to date.”
Huntington Hospital’s caseload stayed above the century mark Wednesday, rising to 107 Covid-19-positive patients. 69% were unvaccinated. 12 of these patients, of whom 83% were unvaccinated, were being treated in the hospital’s ICU.
Across LA County but outside Pasadena health officials reported 40,452 new positive COVID tests and another 39 deaths associated with the coronavirus Wednesday, as the Omicron variant continues to spread across the county.
The 39 fatalities are the highest number of new deaths since Sept. 22.
Of the 36 deaths for which the Los Angeles County Department of Public Health has full data, 78% were among those 65 years of age and older. All deaths occurred in January, likely reflecting an increase in deaths associated with the higher December case and hospitalization numbers.
Wednesday’s test positivity rate was 20.4%.
As more students and staff returned to in-person learning this week amid the surge in cases, routine testing at schools across many districts identified thousands of students and staff infected with COVID-19.
For the week of Jan. 3 through Jan. 9, 547,466 tests were administered across school districts in the county, with most testing occurring for LAUSD students and staff. Last week, 80,424 positive cases were identified, including 68,560 cases among LAUSD staff and students, resulting in a test positivity rate of 14.6%.
A total of three outbreaks among youth sports teams were also identified last week, with an additional 26 school-related outbreaks still being monitored.
“As schools reopen countywide, we are seeing a high number of students and staff testing positive reflecting the explosive rate of community spread,” Public Health Director Barbara Ferrer said.
“Given the importance of ensuring that our schools remain safe for in- person learning, layering in protections is a most sensible approach. Masking indoors and in crowded outdoor spaces reduces transmission opportunities; testing those who are close contacts of infected students or school staff can quickly identify others who may now be infected, and limit continued spread; and, making it easy for those eligible to get their booster doses helps ensure that immune systems are best primed to repel the virus.”
There were 3,912 people with the coronavirus in county hospitals, according to the latest state figures released Wednesday, up from 3,766 the day prior. Perhaps more alarming is a recent spike in the number of those patients in intensive care, which rose from 513 Tuesday to 536. That’s an increase of over 200 people in the last eight days.
However, Dr. Christina Ghaly, the county’s health services director, has said that despite rising patient numbers, the Omicron-fueled surge is playing out differently in hospitals than earlier surges. She said last fall, about one-third of COVID patients wound up in ICU care, but that number is only about 10% to 15% this time around, at least in the four county-operated hospitals, which likely reflect conditions in other medical centers.
She also said that about 40% of COVID-positive patients at the county hospitals were admitted specifically because of the virus, while the rest only learned they were infected upon admission for something else. During the last surge, 80% to 90% of the COVID patients were admitted due to virus-related illness.
Ghaly said current staffing shortages are creating more critical conditions at hospitals. She pointed to large number of health care workers who have retired or moved into non-front-line positions. She also noted that the surge in COVID infections has also impacted health care workers, leaving many unavailable to work due to illness or exposure.
The situation has also led to longer ambulance response times, in part due to large numbers of workers at private ambulance companies who have failed to meet COVID vaccination requirements, leaving them unable to work, combined with a high amount of people calling in sick.
Ferrer has urged residents to avoid dangerous activities in the coming weeks, particularly those that are indoors and involve mingling with unvaccinated or higher-risk people.
She also stressed that while the Omicron variant is easily capable of infecting vaccinated people, the shots are still proving to be effective in preventing infected people from winding up hospitalized.
She said unvaccinated people are nine times more likely to be hospitalized than fully vaccinated people, and 38 times more likely to be hospitalized than people who are fully vaccinated and received a booster shot.
Health officials have said previously that about 90% of people who died from COVID-19 had underlying health conditions. Of the 13 deaths reported Monday, nine had underlying conditions, according to the county Department of Public Health.
The record number of new cases in recent days seems driven in part by a major increase in testing.
On Wednesday, Gov. Gavin Newsom visited a testing site in south Los Angeles County to highlight his COVID-19 emergency response package. On Saturday, Newsom proposed $2.7 billion in new COVID spending as part of his next budget proposal, including a $1.4 billion emergency appropriation request to bolster testing capacity, accelerate vaccination and booster efforts, support frontline workers, strengthen the health care system and “battle misinformation.”













 0 comments
0 comments


