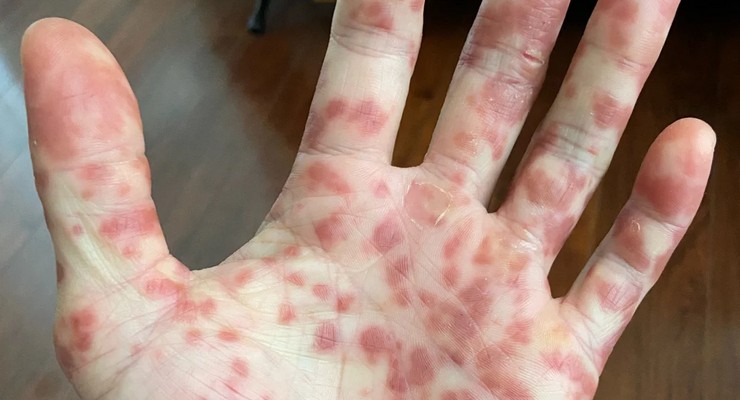
It took multiple telehealth appointments, and trips to urgent care clinics and emergency rooms before an infectious disease specialist diagnosed Kevin Kwong with monkeypox. “Depending on where I was with my symptoms, and who I was speaking to, I was getting different answers,” Kwong recalls. [Courtesy of Kevin Kwong via Kaiser Health News]
Two days after Kevin Kwong flew home to California from New York, his hands itched so badly, the pain jolted him from sleep. He thought the problem was eczema.
“Everything started rapidly getting worse,” the Emeryville, California, resident said. “I started to get more spots, on my face, more redness and they started leaking fluid. The rash expanded to my elbows and my hands and my ankles.”
It took Kwong, 33, six virtual appointments with doctors and nurses, one call to a nurse hotline, a trip to an urgent care clinic, two emergency room visits, and two incorrect diagnoses before an infectious disease specialist diagnosed him with monkeypox in early July.
Despite taking two tests, he never tested positive.
As the number of monkeypox cases has exploded in the U.S. in the past month, the public health system is struggling to spread the word about the virus’s danger and distribute a limitedsupply of vaccines to vulnerable people. But the problem extends even further. People who may be infected are grappling with dead ends, delays, incorrect diagnoses, and inappropriate treatments as they navigate an unprepared and ill-informed health care system.
The once-obscure virus has hospitals racing to teach emergency room staffers how to correctly identify and test for it. Dr. Peter Chin-Hong, the infectious disease specialist at the University of California-San Francisco who ultimately diagnosed Kwong, said his case was a tipping point for the research hospital.
“Kevin came in the middle of the night when a lot of resources weren’t available. So I think after his case, we’re doing a lot more education of the general condition. But I think your average clinician doesn’t always know what to do,” Chin-Hong said.
Monkeypox is caused by a virus in the same family as smallpox, though it’s not as transmissible or fatal. Typically, patients have a fever, muscle aches, and then a rash on their face, mouth, hands, and possibly genitals that can last for several weeks.
The current outbreak is spreading via human-to-human contact, such as touching a lesion, or exchanging saliva or other bodily fluids. People can also become infected by touching objects or surfaces, such as sex toys or sheets, shared with someone with the illness.
The first U.S. monkeypox case of this outbreak was reported May 17, and since then, the number has grown to more than 6,300 probable or confirmed cases representing almost every state, plus Washington, D.C., and Puerto Rico.
California Gov. Gavin Newsom on Monday declared a state of emergency to coordinate response and bolster the state’s vaccination efforts. About half of California’s 1,135 monkeypox cases have been concentrated in the San Francisco Bay Area.
Although anyone can get infected, the outbreak appears to have largely affected men who have sex with men. Kwong said he likely contracted monkeypox from a sexual encounter during New York Pride events.
“This is the first-ever multicontinental outbreak, so it’s not just going to vanish,” said Andrew Noymer, an associate professor at the University of California-Irvine who studies infectious diseases.
“This is not going to blow up like covid, but this outbreak is going to have legs,” he said. “It may be like syphilis and it’ll just sort of be around.”
But most doctors don’t know how to recognize it. In late June, when Kwong began experiencing symptoms, most of the doctors and nurses he spoke with during virtual visits didn’t even mention monkeypox. That doesn’t surprise Dr. Timothy Brewer, a professor of medicine and epidemiology at UCLA.
“Even though I’ve worked on and off in several sub-Saharan African countries over the last 25 years, I’ve actually never treated a case of monkeypox,” Brewer said. “Before this current outbreak, monkeypox was a very unusual disease.”
A rash limited to the genital or rectal area may be mistaken for a sexually transmitted infection. But even if doctors haven’t been trained to recognize monkeypox, Brewer said, their advice to patients could help contain the spread.
“You would be advising people to not engage in sexual activity until their lesions are healed and treated,” Brewer said.
Although many cases are mild and resolve on their own, some rapidly become serious — like Kwong’s.
“Your body is being taken over by this thing that you don’t understand. And you have nowhere to go, so it’s both painful and terrifying,” Kwong said.
Kwong initially treated the rash with the topical steroids he uses for eczema. When that didn’t work, he attended an online appointment with a nurse who diagnosed him with herpes and prescribed an antiviral medication.
Over the next few hours, the rash quickly spread to more of his body. Alarmed, Kwong went to an urgent care clinic. The doctor agreed with the herpes diagnosis, and added another: scabies, a rash caused by mites that burrow into skin. “My spots were concentrated on my hands and my wrists and feet and elbows, which are prime locations for scabies,” Kwong said.
The urgent care doctor had considered monkeypox but Kwong’s spots were clustered together and looked different from the monkeypox rash pictures the doctor had seen. “Depending on where I was with my symptoms, and who I was speaking to, I was getting different answers,” Kwong said.
Over the July Fourth holiday weekend, Kwong frantically reached out to anyone he thought could help as his symptoms worsened.
“I tried to contact doctors, I knew friends of friends who were dermatologists,” he said. “After each time I spoke with someone, I just got rapidly worse. And it was really freaky.”
During another virtual appointment, in the middle of the night, a nurse noticed the rash had spread toward his eyes and told him to go to the emergency room immediately. It was there, at the Alta Bates Summit Medical Center in Oakland, that doctors said Kwong may have monkeypox.
“They were researching while I was in this room, and back-and-forth on the phone with the CDC. I expected myself, as a patient, to be in the dark, but I didn’t realize how little information was also given to providers and how unprepared they were as well,” he said.
He spent 12 hours in the emergency room, where nurses swabbed his lesions for a monkeypox test. They told him to come back if he developed a fever or started vomiting.
“At this point, I was just miserable. I had sores in the back of my throat, in my mouth, all over my body,” he said. “I was just delirious because I couldn’t sleep more than an hour or two at any given time.”
Later that night, Kwong decided to make the trip to the University of California-San Francisco Medical Center. He’d heard through a friend that UCSF Health was treating monkeypox cases, and a virtual care nurse had urged him to go.
When he arrived, he was separated from the other patients, received oxycodone for pain, and was swabbed for another monkeypox test.
The next day, Chin-Hong started treating Kwong for monkeypox. “I thought, wow, this is really, really extensive disease,” Chin-Hong said. “I’ve seen other cases of monkeypox before, but they’re very limited. I would say Kevin is probably in the top 5% of severity of diseases.”
Because the rash was close to Kwong’s eyes, Chin-Hong feared he could go blind if the disease were left untreated. He prescribed Tecovirimat, an antiviral medication branded as TPOXX, that has received special clearance from the FDA to treat monkeypox in certain circumstances.
After the first day on the drug, Kwong noticed that his rash stopped spreading. Over the next two days, the hundreds of swollen spots flattened into red disks. “I was shocked by how fast Kevin improved. It was almost like he was a turbo-rocket on the way to recovery,” Chin-Hong said.
As Kwong started to heal, he got his first test result back: negative. Then the second: negative.
Chin-Hong said health workers might not have rubbed his lesions hard enough to get live cells for the monkeypox test. “It’s very difficult as a clinician to really get a good sample in these kinds of lesions because the patient is often in pain. And you don’t like to see people suffer,” Chin-Hong said.
Cases like Kwong’s may be missed if tests aren’t conducted correctly. The Centers for Disease Control and Prevention’s online resource for clinicians is adequate, Brewer said, but only if you take the time to read all 59 pages.
Clinicians need to collect at least two samples from multiple locations on the patient’s body, he said. The key, Brewer said, is to sample lesions “at different stages of development” and not concentrate only on the early bumps.
For two weeks, Kwong took six antiviral pills a day to rid his body of the virus. He no longer needs pain medication. “My face was the first to heal, which I think helped me a lot, to be able to recognize who I was in the mirror again,” Kwong said.
Now more than a month since the ordeal began, Kwong’s hands and feet are finally healing. His cuticles and the skin on his hands peeled off and are in the process of regrowing, while his fingernails have turned black and started to fall off, he said.
Kwong said the psychological toll will take longer to overcome. “I feel less invulnerable, because it was such a rapidly debilitating disease. And so I’m still working on my mental state more than my physical one.”
This story is part of a partnership that includes KPCC, NPR, and KHN.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.