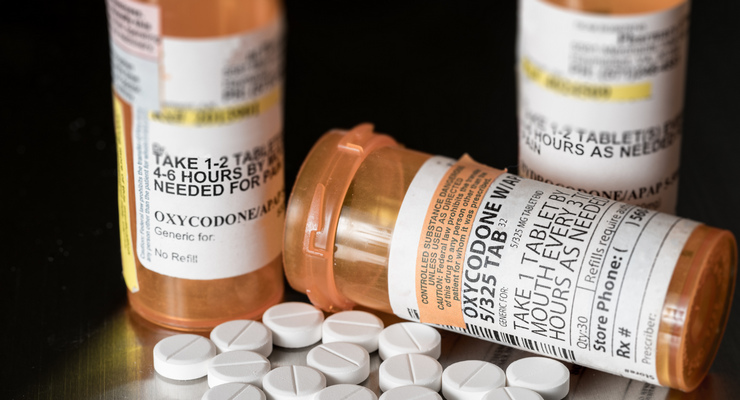
photo credit: Shutterstock
While a rising number of local Fentanyl overdose cases have made headlines in the local news lately, it doesn’t mean that similar cases haven’t been happening for months and even for years, experts say.
This last week saw four deaths from a wave of overdoses in Pasadena.
“All of us at Huntington Hospital are grieving for those affected by the recent opiate overdoses in Pasadena and surrounding areas,” the hospital said in a statement. “These tragic events remind us of the massive toll the opioid epidemic has inflicted on communities across the country.”
“Most of the cases are accidental,” said Clifford Feldman, medical director for psychiatry at Huntington Hospital, because a lot of other drugs are being laced with fentanyl, which is a very, very potent opioid. People don’t know it’s in there, or don’t know how much is in there — they take their usual hit of whatever they take, and they end up not breathing.”
Feldman also explained that Huntington Hospital maintains a virtual intensive outpatient program (IOP) program for such patients who have been detoxed, and are working to remain clean and sober.
The Della Martin Center at Huntington Hospital also offers virtual group therapy for those wishing to maintain their sobriety.
Patients meet three days a week for group and dual diagnosis counseling, he said.
According to Dr. Feldman, some patients have a dual diagnosis, which means they struggle with substances and they have a mental health diagnosis. Huntington Hospital offers hope to both types of people in its virtual outpatient program.
As with many other types of psychiatry issues and conditions, the word “cured’ is a difficult term in this kind of illness because it’s common to have relapses and recurrences,
“Being clean and sober is a daily struggle,” Feldman said.“
Once you are detoxed,” said Feldman, “and you want help initially staying clean and sober, that’s what the program is for.”
As Dr. Feldman explained the length of a patient’s stay in the program is based on three factors.
Since the program is voluntary, the patient’s own desire, or how long they feel they need to be in the program, is one element. The second element is what the treatment team thinks is best for the patient.
And of course, noted Feldman, the third element “that can’t be ignored” is the insurance coverage, or how long the insurance will allow the patient to be in there under their coverage.
Feldman explained that a patient can have insurance and not have mental health coverage, or have mental health coverage and not have substance abuse coverage.
Meanwhile, the nation has seen a rise in hospitalizations cases from marijuana. According to Dr. Feldman, marijuana today is “extremely potent and it’s ingested in extremely efficient ways, like vaping.”
Said Feldman, “In the past, where people would smoke marijuana and it wouldn’t cause a hospital admission, nowadays, when you’re vaping oils and waxes, it makes you sometimes insane. And you end up in the hospital using hospital resources just for marijuana.”
In addition, he said, “The use of methamphetamine is ubiquitous and has skyrocketed like you can’t imagine. I would say that a good portion of the ‘psychiatric patients’ in the emergency room have used methamphetamine within the prior 12 hours.”
There is help available to those who are suf ering from addiction. The Substance Abuse and Mental Health Services Administration (SAMHSA), a division of the US Department of Health and Human Services, has a 24/7 hotline if you or a friend/family member needs somewhere to turn to help with addiction and recovery. SAMHSA’s national helpline is 1-800-662-HELP (4357).
Detox crisis help is available through Huntington Hospital at 800-662-HELP.
To learn more about the Della Martin Center at Huntington Hospital, please call (626) 397-2323